Important Note: This information is constantly changing. Kati Kleber wrote this on March 18-19, 2020, with the most current information available from the CDC at the time. Information may now be outdated. Kleber has attempted to translate what the CDC states as recommendations into easy-to-understand terms for the bedside nurse to get more context behind what’s going on at the national level with COVID-19 preparedness that was accurate at the point of publication. Many of the citations that were current during the writing of this article are no longer active links and have, therefore, been removed.
Anything your organization tells you to do supersedes this information. This is informational only. Any actions you take based upon this blog post are of your own free will and you agree to hold the author harmless. For more information on FreshRN® disclaimers, click here. There is a full reference list at the conclusion of this article.

So much is going on and changing so fast, and I’m seeing a lot of misinformation and fear within our community and want to be able to offer some clarity and support.
First off, the best place for the most up to date information on Coronavirus transmission prevention is the CDC’s website. However, when you get to the site there is a LOT OF INFORMATION! It is really hard to sift through it all to see what’s important.
Well, never fear nurses – I’ve got you! I took some time to check out the current resources and am going to give you an abbreviated version.
Where PPE recommendations ultimately come from
It’s really easy to hop on social media and scroll past scary graph after scary graph, but I encourage you to keep your eye on the prize and head in the game – keeping yourself and your patients safe. There are four places I recommend looking at only and sticking to their recommendations.
- The Center for Disease Control and Prevention
- The World Health Organization
- The American Nurses Association
- Your healthcare organization’s policies, procedures, and communications
The recommendations coming from the CDC, WHO, ANA and have been released with careful consideration, research, and thought from many experts. If you look at all of them and they currently are in line with what your organization is recommending, I encourage you to rest in that reassurance.
As I write this, the CDC, WHO, and ANA are all in agreement with what we should be doing at the frontlines. If your organization is also in line with that, I again encourage you to rest in that reassurance.
I know it’s infuriating and scary to be told airborne precautions one day, and droplet precautions the next… add on to that the constant updates, frightening headlines, existing mask shortage … and all of these very real issues that we’re grappling with…
Know that nation-wide innovative efforts are being made to combat that.
Know that many experts around the world and in the United States agree that N95 respirators and airborne precautions are only necessary when COVID-19 patients are actively producing aerosols during medical procedures, like intubation.
Know that for the vast majority of patient interaction, facemasks and droplet precautions are perfectly appropriate.
The fear of the unknown is very real and palpable. I know it’s probably really challenging and frustrating to be told one day to use airborne precautions and the next that droplet is all that’s needed. I am sure you just want to feel safe and feel respected as a fellow human going to work. At the end of the day, that’s all I would want.
The rest of this article explains the current PPE recommendations and the rationale behind it.
How COVID-19 is spread
In my last post, I discussed how this is a new strain and we’re constantly learning new things about it. As of today (March 19, 2020), both the Center for Disease Control and Prevention and the World Health Organization recommends that COVID-19 positive patients are placed on Standard & Droplet Precautions.
Now, because there is the possibility of aerosolized transmission during aerosol-generating procedures, they’re both recommending having the patient in a negative pressure airborne precautions room if that is anticipated. Otherwise, a regular room with the door closed would be appropriate.
Examples of aerosol-generating procedures include:
- Positive pressure ventilation – BiPAP and CPAP
- Endotracheal intubation
- Airway suction
- High-frequency oscillatory ventilation
- Tracheostomy
- Chest physiotherapy
- Nebulizer treatment
- Sputum induction
- Bronchoscopy
From the CDC:
“Known or suspected COVID-19 should adhere to Standard Precautions and use a respirator or facemask, gown, gloves, and eye protection. When available, respirators (instead of facemasks) are preferred; they should be prioritized for situations where respiratory protection is most important and the care of patients with pathogens requiring Airborne Precautions (e.g., tuberculosis, measles, varicella).” (Emphasis added.)
From the World Health Organization:
“WHO developed its rapid guidance based on the consensus of international experts who considered the currently available evidence on the modes of transmission of 2019-nCoV. This evidence demonstrates viral transmission by droplets and contact with contaminated surfaces of equipment; it does not support routine airborne transmission. Airborne transmission may happen, as has been shown with other viral respiratory diseases, during aerosol-generating procedures (e.g., tracheal intubation, bronchoscopy), thus WHO recommends airborne precautions for these procedures. For more information about healthcare worker protection for 2019-nCoV, click here.” (Emphasis added.)
I also really like this explanation from the University of Chicago Medicine. Below is an excerpt:
“In infection control, we draw a line between things that are transmitted by traveling in the air briefly in respiratory droplets and things that are actually aerosolized and float around for a while. Think of droplets as small bits of fluid that you can feel and see when someone sneezes. You sneeze or cough and these droplets get on surfaces and then you touch them and get them on your hands, or they can fly right into your mouth or nose or eyes. That’s how most coronaviruses are transmitted and that’s how we think this one is too.
Aerosols are different. Think of hairspray after you use it in the bathroom. When you go back to the bathroom later, you may still be able to smell it because it’s lingering in the air. Obviously, we’re learning a lot about this virus, but most coronaviruses aren’t airborne that way. Generally speaking, there may be times when some of these droplets or particles are airborne, but it’s limited.”
Again, because this is a new strain, we’re not 100% sure about the intricacies of its transmission. But we have been dealing with coronaviruses since the 1960s, and they are thought to be responsible for about 15-30% of respiratory tract infections annually.
While this strain of coronavirus has been detected in different clinical specimens (upper and lower respiratory tract, blood, stool, etc.) the duration in which it’s viable and can be spread to other people is unknown. Just because something is detectable doesn’t mean it’s also viable. It’s also unknown if the infectious virus is present in extrapulmonary specimens (pleural fluid, pericardial fluid, swabs, etc.) or in non-respiratory fluids (breast milk, urine, vomit, stool, etc.) can have the ability to transmit it either (source).
Now, a study was released just this past week which evaluated how long the virus remained detectable in five environments: aerosols, plastic, stainless steel, copper, and cardboard.
They found that the aerosols remained detectable for at least 3 hours. On stainless steel or plastic, the viable virus remains after 3 days, on cardboard, it is not viable after 24 hours, and on copper, it’s inactivated after 4 hours (source).
Please note, those findings should be interpreted with extreme caution, as this only one experiment. It has not been peer-reviewed, replicated by another group, and is examining the virus in the ideal setting with a lot of the virus. This article explains why this should be interpreted with extreme caution.
The article also states that the WHO is aware of this emerging data and studied it to see if they should change their current recommendations. (To refresh, their current recommendation is DROPLET precautions normally, and if the patient is going to have procedures where they will generate aerosols, those AIRBORNE precautions are used.)
WHO technical lead for the COVID-19 response, Maria Van Kerkhove, stated, “From the available studies that we have seen, we are confident that the guidance we have is appropriate.”
Please see the following excerpt from that article:
The weight of the evidence suggests that the new coronavirus can exist as an aerosol — a physics term meaning a liquid or solid (the virus) suspended in a gas (like air) — only under very limited conditions, and that this transmission route is not driving the pandemic. But “limited” conditions does not mean “no” conditions, underlining the need for health care workers to have high levels of personal protection, especially when doing procedures such as intubation that have the greatest chance of creating coronavirus aerosols. “I think the answer will be, aerosolization occurs rarely but not never,” said microbiologist and physician Stanley Perlman of the University of Iowa. “You have to distinguish between what’s possible and what’s actually happening.”
The article continues to state:
“If it could easily exist as an aerosol, we would be seeing much greater levels of transmission,” said epidemiologist Michael LeVasseur of Drexel University. “And we would be seeing a different pattern in who’s getting infected. With droplet spread, it’s mostly to close contacts. But if a virus easily exists as an aerosol, you could get it from people you share an elevator with.”
According to the Centers for Disease Control and Prevention, that is not happening. Earlier this month, CDC scientists reported that the rate of symptomatic infection among a patient’s household members was 10.5%. The rate among other close contacts was 0.45%. In the case of one particular patient, none of his five household members, although continuously exposed to the patient during the time he was isolated at home, tested positive for the virus.
Again, here is a link to that specific article – one of which I’d recommend reading in its entirety.
Another paper from JAMA was published, citing and confirming that droplet was the main form of transmission. Additional research confirms that coronaviruses have quite a bit of difficulty existing in the aerosolized form in warm, humid conditions.
Essentially, top international experts agree that while the coronavirus can exist in an aerosolized environment, it’s clearly not the main form or how routine transmission occurs. Otherwise, we would be seeing substantially larger numbers of cases, particularly in those individuals who have shared close (like in the same home) contact with infected individuals.
Main concerns of the healthcare community on COVID-19
From reading articles, social media, and personally speaking with many, the main concerns appear to be:
- Having enough personal protective equipment for themselves and patients – in particular masks and ventilators
- Knowing the appropriate way to prevent transmission so providers themselves don’t get sick
Because of the public fear and hysteria around this, the public is buying up stocks of their own masks, sanitizer, and other protective equipment. The trouble is, the general public can go home and self-isolate. Health providers cannot. We must be at the front lines taking care of the patients, therefore it is more important for health care providers to have masks and other forms of personal protective equipment than the general public.
Manufacturers are having trouble keeping up with demand. Even if they get everything made quickly, it still must be physically delivered to the hospital, then distributed out to the staff. Add to that all of the many shutdowns and changes in normal processes, we’re seeing nurses re-using their own masks, using different kinds of masks because something is better than nothing, having to hide boxes of masks in the nurse’s station because the public is stealing them, and health care providers quarantining themselves so they don’t get their own families sick.
When you don’t have what you need to keep yourself safe while taking care of a patient with an infectious disease – that’s pretty scary.
On March 18, 2020, President Trump met with nurses to discuss the major concerns of lack of appropriate PPE. Here is the video, here is the transcript, here is the ANA press briefing summary. Essentially, they’re trying various innovative methods to get more masks ASAP (like ordering an immediate increase in production, construction companies donating their masks, DOD releasing masks, etc.)
Lowering our risk as much as possible before putting on PPE
Whenever we’re taking care of someone with an infectious disease, there are multiple things we must do as healthcare providers to lower our risk of getting it ourselves. The overall goal is to provide care to the patient while keeping ourselves safe. However, we tend to look at the PPE as our only means to keep ourselves safe, when that is really just the tip of the iceberg.
We want to control our exposure to occupational hazards as much as possible. There’s actually an engineering hierarchy to this. See the below diagram, directly from the CDC.
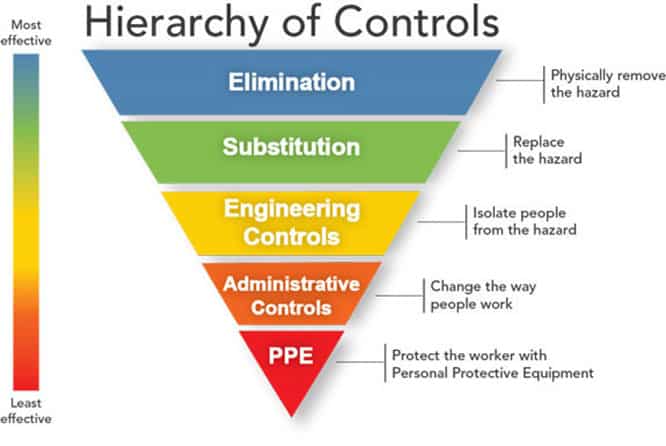
Source: Center for Disease Control and Prevention (link)
We can physically remove the hazard by making any COVID-19 patient who does not require hospital care go home to self-quarantine. The issue is, for us on the front lines, we’re mainly working with the orange and red methods of protection because we must physically care for the patient.
However, we can drastically reduce our likelihood of exposure by isolating the patient (yellow) and changing how we work (orange) before we even put on PPE.
To use a less-than-perfect analogy, to prevent getting injured in a car accident, we don’t just put on a seat belt and drive recklessly. We do a lot of things to prevent accidents and to keep ourselves and others safe.
We make sure the car is in good condition itself, we drive safely, avoid hazardous situations, remove distractions, and when we’re in areas of increased risk (like on highways driving at higher speeds), we increase our level of awareness because minor mistakes going at 70 mph are a lot more detrimental than the same lapses or mistakes at 25 mph. And we wear our seat belt through all of it.
PPE is kind of like a seat belt. It’s always necessary when dealing with patients who have a communicable disease, but it’s only part of being safe – not the only level of protection we’ve got.
Going back to our colorful diagram, if you look at the yellow and orange areas, there is a lot there that can substantially reduce our risk of transmission.
Examples of maintaining that isolation (yellow/engineering controls) include:
- Having a specific area of the unit/hospital for COVID-19 patients
- Having the patient in a private room with appropriate air ventilation, keeping the door(s) closed
- Only allowing specific personnel in the room with them and restricting visitors/non-essential points of patient contact
Examples of administrative controls (orange) for taking care of these patients include:
- Staying 6 feet away as much as possible while in the room (so if you’re not actually touching them, staying back)
- Clustering care
- Only physically touching the patient when you absolutely have to
- Not charting at their bedside
- Adding additional barriers (like a curtain)
- Using a video monitor with the patient, so that if you just need to ask them a question you can do so without using another mask and getting physically near the patient
Administrative controls are highly effective in protecting healthcare workers and should not be overlooked (source).
After we’ve done all we can to implement these isolation and administrative controls, now we start talking about personal protective equipment, or PPE. We all know that as nurses we must touch the patient and will definitely need PPE, but if we can do all that is within our power and judgment to wisely use it when we need it, and maximize our efforts with isolation and administrative controls, we can significantly reduce the amount of PPE used and drastically increase our own safety.
Again, I think a lot of weight gets put on PPE to be the only thing keeping us safe, but really these other methods are just as important and when combined are incredibly effective. Many of us tend to gown and glove up, toss on a face mask and think we are 100% safe. We need to also wash hands appropriately, have our PPE on correctly, and be mindful of the actual physical interaction.
If we’re doing a bed change, that means we’ve got the supplies we need and we’re not going in and out of the room multiple times… we’re being cautious while physically cleaning… we’re being cautious about how we’re disposing of material… we’re putting a face mask on the patient if we have to speak to them or get all up in their business… if patients are vented or need to be intubated, only 100% essential personnel are in the room and all have the appropriate PPE and you’re in a negative pressure room… and so forth.
It can be easy to get relaxed and comfortable at the bedside and subsequently be less diligent in protective measures because PPE does make you feel safe. It’s this physical barrier that makes it feel like you can continue on, business as usual, with patient care.
But, this isn’t business as usual.
I know we want to provide the exact same care for our isolated patients as patients who are not on isolation. That is absolutely true; however, during times where we are faced with a communicable disease and we’re low on supplies, we need to make appropriate adjustments to enable us to continue to provide care to our entire patient population while keeping ourselves safe.
I know it can feel weird or almost like betraying your beliefs on how you should care for your patients (because everyone, regardless of what’s going on, should get the same quality of care), but this is a very unique situation. Lingering to have a 40-minute conversation with a coughing COVID-19 patient would not be wise right now… nor would allowing 4 students to watch a COVID-19 patient get intubated… or charting at the bedside for 35 minutes while the snoring COVID-19 patient is 24 inches from your left shoulder.
So, what if we run out of masks?
The CDC actually has a document on its website called Strategies for Optimizing the Supply of N95 Respirators, and they break it down into three levels. This page is very well organized and if you’ve got time, I recommend checking it. You can go to each level and see the corresponding engineering and administrative controls (please note, all of the following information will come from that page or an extension of it).
Let’s go over the three levels outlined by the CDC of dealing with a short supply of masks.
I think of this as our color-coding: green, yellow, and red. (The CDC doesn’t use that color coding, that’s definitely the way it makes the most sense in my Kati Kleber brain.)
Conventional
This means that there are no changes in daily practices and how your hospital normally functions day-to-day. We’re not being wasteful with our masks and only using them when indicated. This truly is business as usual.
Contingency
Changes are made, but they may not have a significant impact on the care to the patient. Decisions are made on a case by case basis, taking multiple factors into account (source). These factors can include things like the number of respirators available, usage rate, etc.
Here is the link for the following information.
Examples of interventions for this level
- Using N95 respirators beyond the manufacturer-designated shelf life for training and fit testing. This means that the people who are fit testing everyone are not grabbing brand new ones to test people, they’re using these masks past the shelf life to save the fresh ones for people actively caring for those patients.
- Extending the use of N95 respirators. They define “extended use” by saying you can wear the same N95 mask for repeated close contact with several patients with the same diagnosis. So, if you were caring for 2-3 COVID-19 patients in the same unit, you could keep the same mask on (without taking it off) for caring for those specific patients. The decision to do this at your specific organization must be made by administrators who manage respiratory protection, occupational health, infection control, and even requiring input from state/local public health departments. This isn’t something nurses should do on a whim. If it is being communicated to you to do this by the administration, it was not a decision made lightly and most likely required a lot of thought, planning, and input.
- Leveraging limited reuse of N95 respirators. So, limited reuse and extended use are different. In terms of limited reuse, this would mean reusing the same N95 mask for the multiple patients, but taking it off after each encounter with a maximum of 5 uses per device to ensure an adequate safety margin (source). Masks should not be shared by different health care providers with one another, and in between uses the mask should be stored in a manner so it won’t get compromised (like leaving it on a counter for it to get wet… it should be hung up or in a bag, etc.).
(Interestingly, the CDC does mention that for pathogens where contact transmission isn’t a concern (like TB), routinely limited re-use has been practiced for decades. You can reuse that same single-use N95 mask up to 5 times per patient as long as the mask itself retains its function and structural integrity. Now, this would not apply to COVID-19 patients, but does offer some insight on standard acceptable practices with different pathogens.)
To summarize those two points:
- Extended use = keep it on for a longer period of time without taking it off, even while caring for different patients (but ones that have the same pathogen, like multiple COVID-19 patients)
- Limited reuse = taking the mask off after each encounter, but reusing the same mask up to 5 times
Crisis
This level is not at all routine and the decision to implement these practices are made with very careful and serious consideration along with the local healthcare coalition, as well as state, federal, or local public health officials, and any other appropriate agencies managing the local response to COVID-19. Needless to say, the decision to move into “crisis mode” isn’t taken lightly, and many people are involved in this.
They break this out into two sections: When supplies are running low and when there are none left. Here is the link that explains each of the following situations in greater detail.
When N95 supplies are running low
The things that the administration may instruct you to do when N95 are running low include:
- Using respirators beyond shelf life. They all have a shelf life (meaning the length of time the manufacturer can guarantee its efficacy), but if there is a stockpile of N95’s that have expired but have yet to be used, those would be utilized in this case. Here is more information on this.
- Using N95 respirators that are approved in other countries that are similar to the US-approved N95 respirators. Naturally, there are a lot of respirator products out there in the world and other countries have similar processes for approving their devices and they are expected to protect their workers. In crisis situations, these can be utilized as suitable alternatives in the US. On this page, there is a table of 7 different countries with similar acceptable products that compare to the US performance standard.
- Limited reuse of N95 respirators for COVID-19 patients. This is the same measure described previously in “contingency”. Essentially, if you’ve got a COVID-19 patient you’re reusing the same N95 mask up to 5 times, removing it after each patient encounter.
- Use N95 respirators past their shelf life not only for COVID-19, but for TB, measles, and varicella as well. Naturally, this would depend on if you do have other patients at your facility requiring this.
- Prioritizing the use of the N95’s and facemasks by the type of activity. Essentially, when this measure is utilized you’re judging when to use an N95 by each situation. Now, this is an example and may differ so bear with me… If you’re going to be in the room and providing direct care, you may only use a facemask. If your patient requires any of those previously mentioned aerosol-generating procedures (intubation, trach, CPAP/BiPAP), then use your N95’s or other respirators. We’re basically saving our N95 respirators for the times where we are more likely to come into direct contact with the pathogen rather than all the time. There is a table on this page that explains different situations.
When no respirators are left
This would be dire circumstances, but should there be absolutely no respirators left, here is what the CDC recommends organizations should do:
- Make sure healthcare providers who are at a higher risk for illness from COVID-19 are not taking care of COVID-19 patients. Depending on the size of your hospital and nursing units, some hospitals may ask the staff for volunteers to be on a team of go-to people to assign these patients to. (That’s what my hospital did back in 2015 when I was on the Ebola Team.)
- If there are healthcare providers who have clinically recovered from COVID-19 themselves, they would be preferred to provide direct patient care. This is included because there is a possibility these individuals would have developed some protective immunity. (Keep in mind, that is a theoretical assumption and it is not certain that people who have recovered from this strain possess immunity to it.)
- Placing COVID-19 patients in special isolation rooms that have high-ventilation capacity. The thought is by putting a patient in a room that is highly ventilated with negative pressure, in an inner isolation zone within a “clean” larger ventilated zone, that by using those measures with face masks can mitigate the risk of transmission. This isn’t an evidence-based method, but when we’re in crisis mode with no N95’s, this is a measure that is thought to make a difference.
- Using ventilated headboards. Basically, it’s a board that’s placed at the head of the bed that draws exhaled air up into its HEPA filter and therefore decreases the risk of the healthcare provider being exposed to it.
- Using non-approved masks or homemade masks. When we’re down to the wire, we have to place some sort of physical barrier on our faces to prevent possible transmission. This is the last resort and extreme caution must be exercised when utilizing it (so, ensuring ALL administrative and engineering controls have been fully maximized).
Confused yet?
It took me a long time to read through the CDC’s current recommendations for how they recommend healthcare organizations deal with COVID-19.
If it seems like you never see your administrators during this time of crisis, it’s probably because they’re all spending time reading the latest updated information, pulling in local, state, and even federal health officials to make decisions, then communicate those decisions and get supplies.
Again, there is a lot of information out there and some of it can be quite confusing and make it really difficult to know exactly what to do.
My final thoughts, nurse to nurse
Know that the decision to go from airborne to droplet did not come lightly, nor without great thought, research, and consideration from local, state, national, and worldwide entities.
Know that there are many nurse leaders out there advocating on your behalf and palpate the fear and concern.
Know that your safety and expertise matter.
We will get through this, nurses. Keep providing that outstanding patient care you know how to give to these patients. I know it would be completely unacceptable to you to do anything less.
As a society, we again are asking too much of you. I am hopeful that in this storm you are able to find calm, peace, and purpose in helping and caring for those who cannot help themselves.
I see you. I hear you. I honor you in how you are serving humanity at this desperately important time. You are so incredibly valued and I pray you know that deep within your soul.
Stay strong, nurses. We will get through this.
References
- Begley, S. (2020, March 16). The new coronavirus can likely remain airborne for some time. That doesn’t mean we’re doomed. In STAT. Retrieved March 19, 2020, from https://www.statnews.com/2020/03/16/coronavirus-can-become-aerosol-doesnt-mean-doomed/
- Bergman, M. S., Viscusi, D. J., Zhuang, Z., Palmiero, A. J., Powell, J. B., & Shaffer, R. E. (2012, May). Impact of multiple consecutive donnings on filtering facepiece respirator fit. American Journal of Infection Control, 40(4), 375-380. doi:10.1016/j.ajic.2011.05.003
- Center for Disease Control and Prevention. (2020, March 17). Healthcare professionals: Frequently asked questions and answers. In Coronavirus Disease 2019 (COVID-19). Retrieved March 19, 2020, from https://www.cdc.gov/coronavirus/2019-ncov/hcp/faq.html
- Center for Disease Control and Prevention. (2020, March 10). Interim infection prevention and control recommendations for patients with suspected or confirmed Coronavirus Disease 2019 (COVID-19) in healthcare settings. In Coronavirus Disease 2019 (COVID-19). Retrieved March 19, 2020, from https://www.cdc.gov/coronavirus/2019-ncov/infection-control/control-recommendations.html
- Center for Disease Control and Prevention. (2020, February 28). Release of stockpiled N95 filtering facepiece respirators beyond the manufacturer-designated shelf life: Considerations for the COVID-19 response. In Coronavirus Disease 2019 (COVID-19). Retrieved March 19, 2020, from https://www.cdc.gov/coronavirus/2019-ncov/release-stockpiled-N95.html
- Center for Disease Control and Prevention. (2020, February 29). Strategies for optimizing the supply of N95 respirators: Contingency capacity strategies. In Coronavirus Disease 2019 (COVID-19). Retrieved March 19, 2020, from https://www.cdc.gov/coronavirus/2019-ncov/hcp/respirators-strategy/contingency-capacity-strategies.html
- Center for Disease Control and Prevention. (2020, March 17). Strategies for optimizing the supply of N95 respirators: Crisis/alternative capacity strategies. In Coronavirus Disease 2019 (COVID-19). Retrieved March 19, 2020, from https://www.cdc.gov/coronavirus/2019-ncov/hcp/respirators-strategy/crisis-alternate-strategies.html
- Center for Disease Control and Prevention. (2020, February 29). Strategies for optimizing the supply of N95 respirators. In Coronavirus Disease 2019 (COVID-19). Retrieved March 19, 2020, from https://www.cdc.gov/coronavirus/2019-ncov/hcp/respirators-strategy/index.html
- Center for Disease Control and Prevention. (2016, January 7). Transmission-based precautions. In Infection Control. Retrieved March 19, 2020, from https://www.cdc.gov/infectioncontrol/basics/transmission-based-precautions.html
- Chopra, V., Christensen, B., & Janssen, L. (2017). Infection prevention: A hierarchy of control. In Medscape. Retrieved March 19, 2020, from https://www.medscape.org/viewarticle/880302
- Fehr, A. R., & Perlman, S. (2015). Coronaviruses: an overview of their replication and pathogenesis. Methods in molecular biology (Clifton, N.J.), 1282, 1–23. https://doi.org/10.1007/978-1-4939-2438-7_1
- Fishers, E. M., & Shaffer, R. E. (2014). Considerations for recommending extended use and limited reuse of filtering facepiece respirators in health care settings. Journal of Occupational and Environmental Hygiene, 11(8), 115-128. doi:10.1080/15459624.2014.902954
- Hick JL, Barbera JA, Kelen GD. Refining surge capacity: conventional, contingency, and crisis capacity. Disaster Med Public Health Prep. 2009;3(2 Suppl): S59-67. doi: 10.1097/DMP.0b013e31819f1ae2
- Landon, E. (n.d.). COVID-19: What we know so far about the 2019 novel coronavirus. In UChicago Medicine. Retrieved March 19, 2020, from https://www.uchicagomedicine.org/forefront/prevention-and-screening-articles/wuhan-coronavirus
- Parodi, S. M., & Liu, V. X. (2020, March 13). From containment to mitigation of COVID-19 in the US. In JAMA Network. Retrieved March 19, 2020, from https://jamanetwork.com/journals/jama/fullarticle/2763187Tran, K., Cimon, K., Severn, M., Pessoa-Silva, C. L., & Conly, J. (2012). Aerosol generating procedures and risk of transmission of acute respiratory infections to healthcare workers: a systematic review. PloS one, 7(4), e35797. https://doi.org/10.1371/journal.pone.0035797
- van Doremalen, N., Morris, D. H., Holbrook, M. G., Gamble, A., Williamson, B., Tamin, A., … de Wit, E. (2020, March 17). Aerosol and surface stability of SARS-CoV-2 as compared with SARS-SoC-1. In The New England Journal of Medicine. Retrieved March 19, 2020, from https://www.nejm.org/doi/full/10.1056/NEJMc2004973
- The White House. (2020, March 18). President Trump meeting with nurses on coronavirus response. In C-SPAN. Retrieved March 19, 2020, from https://www.c-span.org/video/?470490-1/president-trump-meeting-nurses-coronavirus-response
- World Health Organization. (2020, January 25). Infection prevention and control during health care when novel coronavirus (nCoV) infection is suspected. In Publications. Retrieved March 19, 2020, from https://www.who.int/publications-detail/infection-prevention-and-control-during-health-care-when-novel-coronavirus-(ncov)-infection-is-suspected-20200125
- World Health Organization. (2020, March 1). Q&A on infection prevention and control for health care workers caring for patients with suspected or confirmed 2019-nCoV. In Newsroom. Retrieved March 19, 2020, from https://www.who.int/news-room/q-a-detail/q-a-on-infection-prevention-and-control-for-health-care-workers-caring-for-patients-with-suspected-or-confirmed-2019-ncov


I feel like in the US these gowns and PPE we are wearing is very flimsy. I see nurses wearing regular masks and I just don’t agree with it. The nurses in China are wearing Hazmat suits to care for these patients. We are getting ourselves exposed with these plastic gowns and mask.