Stay calm and remember these tips when your patient codes. This will help you respond quickly and correctly every time. Dealing with a coding patient can be a very scary experience. To ease the shock value, let’s go over some extremely basic steps that you’ll be able to recall even in chaos.
(This post is about responding to adult patient codes and is informational only. Please refer to your hospital’s policies and procedures to guide your practice. Our full disclaimer is here.)
Quick note ➡️ If your patient recently had cardiac surgery (within this admission), how you respond to a code is different. There are resuscitation guidelines specifically for patients who have recently had valve or aneurysm repairs, pacemakers placed, coronary artery bypass grafts, and other serious cardiac surgeries. To learn more about the appropriate emergency response protocols for this unique patient population, click here.

Table of Contents
3 Things To Do When A Patient Codes
There are three very basic things you should do every time a patient codes. Typically, when a code is called, people run into the room, and it is a team effort. The way this list of 3 things to do is structured is that if you come into the room and someone else is already doing #1, go to #2, and so on.
- Check carotid pulse
- If there is no pulse, begin chest compressions
- Secure airway
Remember ➡️ if you check their pulse and they have one, that means that their heart is beating strong enough to create the pulse, which means that chest compressions are not necessary at this time.
Now, if this is one of the first few times that you are witnessing a cardiac or respiratory arrest, you might freeze. Even though you logically know what to do, accessing that information in your brain during a life-or-death emergency is almost impossible during your first exposure.
Our Fight Or Flight Response
As humans, we all have a fight-or-flight response. When we see an emergency in front of us, our body reacts – it is innate. It is not something you are consciously in control of.
If you see someone code and you freeze, it does not mean you are a terrible nurse who cannot do this. It means your body is doing what it was designed to do. Nurses were not born with different brains that don’t have this life-saving mechanism. Instead, our goal as nurses is to train our brains to respond appropriately.
How To Regulate That Response
The first step to change is awareness. Simply being aware that your body will react this way is incredibly valuable.
Next, we want to give the part of our brain responsible for higher-level thinking (our prefrontal cortex) a chance to catch up with the part responsible for detecting and reacting to threats (our amygdala). Our amygdala says, “DANGER DANGER!” and innately responds faster than we are conscious. Once it catches up, the prefrontal cortex will enable you to take the steps you have been taught. Therefore, give it a second to catch up.
The PFC is highlighted in red below.
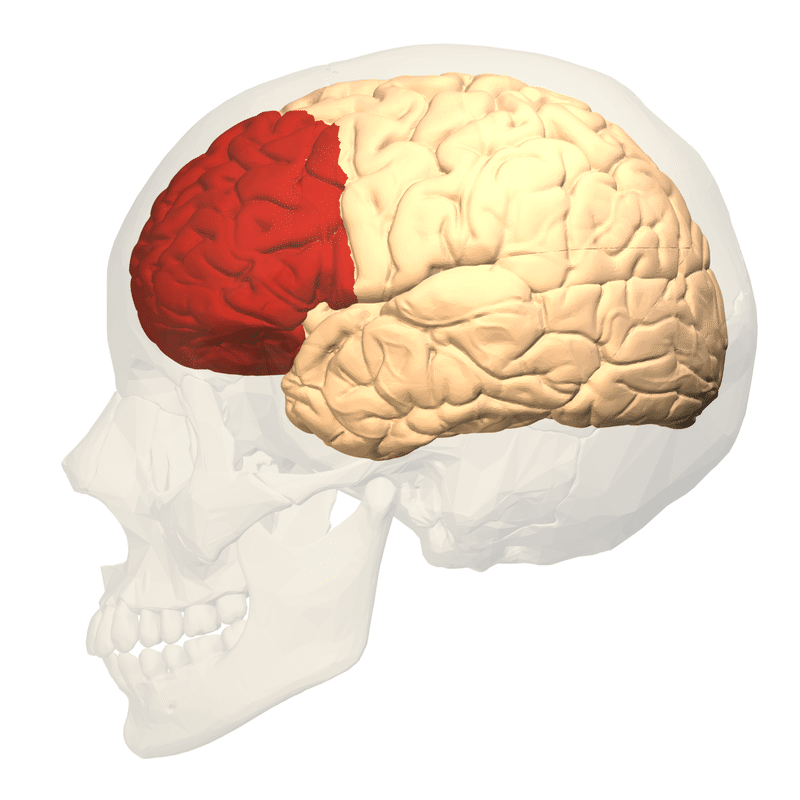
This freeze response reminds me a lot of when a professor or nursing instructor calls on you to answer a question, and your mind goes blank. Then, when the pressure is off, you think, “Man, I knew that answer!”. It’s the same situation, except the stakes are a bit higher.
So, when you feel your body freeze, take a deep breath and remind your brain that you are not in danger. As silly as this sounds, telling yourself, “I’m safe. I’ve got this,” can be all you need to do to lean back into the action. We want to outsmart our brains!
Wish Your 12-Hour Shift Had A Map?👇

This course helps you turn a messy 12-hour acute care shift into a clear, structured rhythm. You’ll learn how to organize your day after report, prioritize when everything feels urgent, recover when something throws you off track, and give a stronger end-of-shift handoff. No fluff, no vague advice. Just a repeatable system you can use shift after shift. Designed specifically for med-surg, stepdown, and ICU nurses who are tired of feeling behind. No fluff. Just practical training you can use on your very next shift.
See What’s Inside Shift OS →
Next, we tend to overcomplicate things. While codes can get complex when we start digging into things like the Advanced Cardiac Life Support (ACLS) algorithms, drugs, and all that, it can also be very simple at the beginning.
Let’s make the interventions so painfully simple that even during those foggy milliseconds, our frozen brain can recall them. Here’s how I want you to simplify our interventions:
- Pulse
- Chest
- Air
Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air. Pulse, chest, air.
Tell yourself that over and over again so that it’s so engrained into your brain that your thoughts can get there when they’re coming out of a freeze-state.
Spoiler Alert: It Requires Repetition
You’ll probably freeze the first few times. Please remember that it is 100% normal and human to do so. The more awareness you have of this natural response, the sooner your brain and body will acclimate to responding promptly in emergencies. You are training your brain to respond to emergencies differently and will need repeated exposure to facilitate this training. This is why people who work in intensive care units and emergency departments.
What Patient Codes Practically Look Like
Let’s walk through an example. While it will take a few minutes to read this, please know that in reality, this will all unfold in a matter of seconds.
When that patient codes, there is typically a response that resembles organized chaos. The code team is trained in ACLS and is used to responding to codes. But, it typically takes them 1-3 minutes to arrive, depending on where your unit is located in the hospital. Therefore, do not focus on learning how to run an ENTIRE code. Let’s focus on what to do before that code team arrives.
Patient Codes Example: Your Patient Flatlines
You’re at the nurse’s station, catching up on charting. You hear the telemetry alarm above your head and see a flatline on your patient. The emergency phone on your unit rings. It’s the telemetry monitor technician who will notify the unit of the code.
You run into the room and are the first person there. The head of the bed is 40 degrees, as the patient was sitting up to eat lunch. They are unresponsive.
You immediately take two fingers, place them on their carotid artery, and do not feel a 🫀 pulse. You scream for the code cart (your team likely has already started to grab that), pull the CPR lever to get the bed flat, and begin compressions. Chances are, you will need to hop on their bed to get the right angle and leverage to push down hard enough.
Full disclosure ➡️ The first time you push down on their chest hard enough to effectively provide chest compressions, you will feel the patient’s ribs cracking under your hands.
Once the Code Cart Arrives
You will continue your compressions while your colleagues are assembling around you. The next person in the room should run to the head of the bed and grab the bag-valve-mask (BVM).
(We go through a code demo and show you what the BVM looks like and even how it works in this course. It is also part of our All-Access Pass)
This nurse should grab the BVM and crank the oxygen up as high as it goes. Then, they will tilt the patient’s head back, lift their chin (a classic head-tilt move!), and place the mask on the patient’s face, covering both the nares and the mouth. Once this person is set up, then you can do your standard 30 compressions to two breaths.
If someone is doing compressions and someone else is in charge of the airway, you are GOLDEN! Someone is beating the patient’s heart for them, and someone is making oxygen go into their lungs.
Miscellaneous Patient Codes Tasks
If someone is on the chest and another person is taking care of the airway and the code team has not arrived yet, here are a few things you can do:
- Get the backboard off of the code cart and be ready to slide it under the patient in between a set of compressions
- Assess IV access; if something non-essential (like an antibiotic) is running through their one IV access point, then flush it and disconnect it to be ready to administer life-saving drugs (or for the code team to do so)
- Pull up the patient’s chart and get the code initiated
- Swap in for the patient’s primary nurse, who will need to speak with the code team physician to provide an accurate history
- Be a runner to grab supplies as they are needed
- Get in line to switch out the person doing compressions during the next break
If all tasks are taken up, then the best thing to do can be to check on other patients to ensure their needs are being met. Notice who the primary nurse is for the coding patient and check on their other patients because that nurse will likely be tied up for a bit.
Final Thoughts on Patient Codes
Remember: if you freeze, it is okay! It doesn’t mean you are a bad nurse or not cut out for this job.
Please have realistic expectations for your development as an acute care nurse. With actively training your brain and body to respond appropriately and ensuring you have repeated exposure to code, you will feel confident and comfortable in them in no time.
More Resources for Patient Codes
- S2E21: Code STEMI, Code Stroke, and Code Sepsis
- S1E3 – What to do During a Code
- S5E41 – When Nurses Should Call the Rapid Response Team
The ICU learning curve is STEEP. Let's make it easier.

Starting in the ICU can feel like drinking from a fire hose. The learning curve is real... but what if you had a head start?
Breakthrough ICU is designed just for new ICU nurses. You’ll get straight-to-the-point guidance on common ICU disease processes and treatments, equipment, report, and time management—so instead of playing catch-up, you’ll feel ready from day one.💪
Start Now!



0 Comments