The middle cerebral artery, or MCA, is the artery most commonly involved in acute ischemic stroke. It supplies a large portion of the lateral frontal, parietal, and temporal lobes, along with deep structures such as the basal ganglia and internal capsule. Because of that territory, MCA strokes can affect movement, sensation, vision, speech, attention, awareness, swallowing safety, and behavior. For nurses, the key is not just knowing the anatomy. It is recognizing the pattern, protecting the patient from complications, and catching subtle worsening early.
This guide will walk you through what an MCA stroke is, the different types of strokes that affect this artery, what causes them, and how nurses can support patients through recovery. (And it’s written by me, Kati Kleber MSN RN, a former neuro ICU nurse and current nurse educator!)

Table of Contents
What Is the Middle Cerebral Artery?
The MCA is one of the three major cerebral arteries, branching from the internal carotid artery. It delivers oxygen-rich blood to the lateral surfaces of the frontal, parietal, and temporal lobes, as well as to deep brain structures such as the basal ganglia and internal capsule. Because the MCA supplies both cortical areas and deep motor pathways, MCA strokes can cause a mix of motor, sensory, visual, language, attention, and behavioral deficits.
Below is an image of the general blood supply of the brain. This view is if you were lying on the floor, looking up at the bottom of the brain.
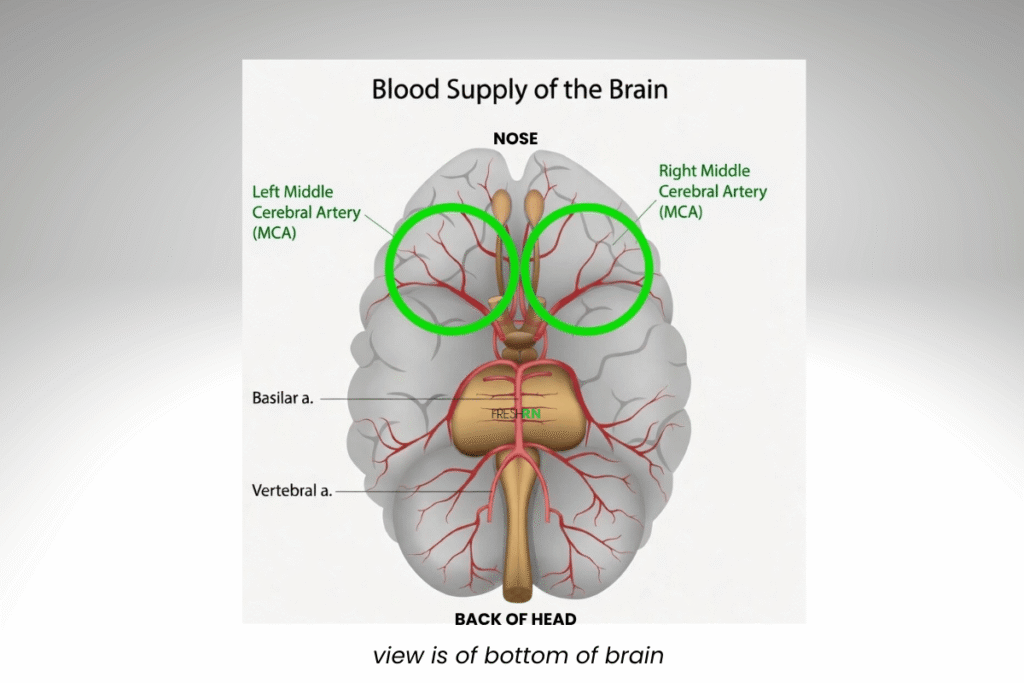
Below is the areas of the brain the MCA supplies, highlighted in RED. This view is if your were looking down at the brain from above, looking at the crown of the head.
Again, notice that there are are two middle cerebral arteries, one on each side.
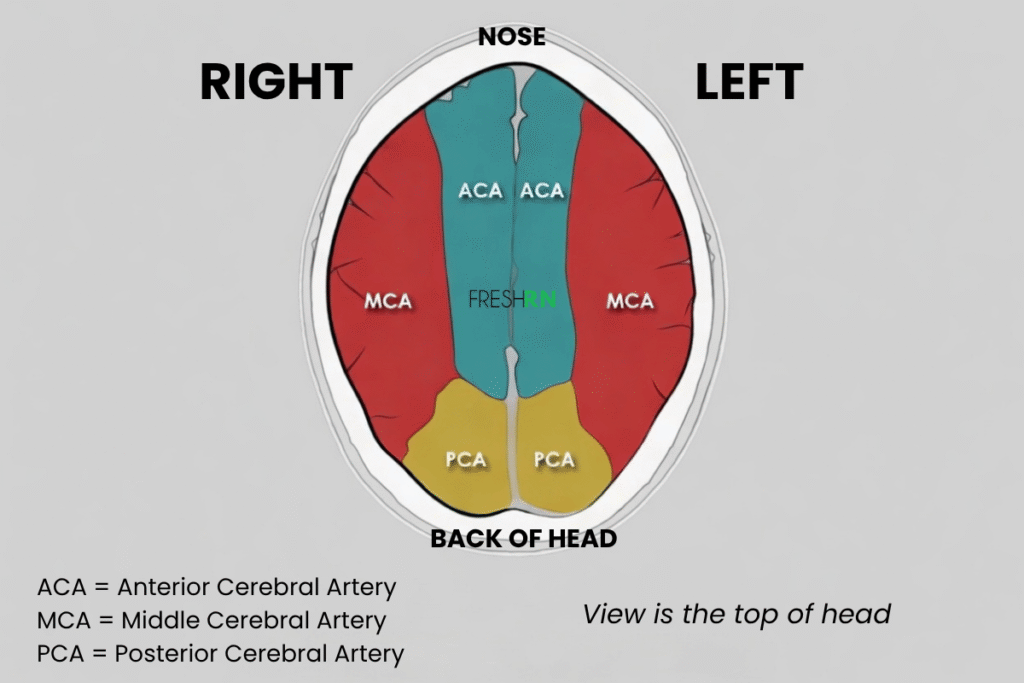
MCA Location Bedside Translation
The MCA is one of the brain’s main blood supply roads.
It branches off from a larger artery in the neck and brings oxygen-rich blood to important parts of the brain. These areas help control movement, feeling, vision, language, attention, and behavior.
That is why an MCA stroke can cause so many different problems. It is not just “one-sided weakness.” Depending on where the stroke occurs, the patient may have trouble moving one side of their body, feeling one side of their body, seeing part of their environment, speaking, understanding language, paying attention, or acting like themselves.
What Is an MCA Stroke?
An MCA stroke most commonly refers to an ischemic stroke in the MCA territory, usually from an occlusion in the MCA itself or from an embolus that travels into the MCA. Less commonly, bleeding from an aneurysm, AVM, trauma, or intracerebral hemorrhage can affect the MCA territory and produce MCA-pattern deficits.
The MCA is divided into four main segments (M1–M4), and symptoms vary depending on which branch is involved. As a result, patients may experience anything from mild motor deficits to profound language loss, depending on the territory affected.
MCA Stroke ➡️ Bedside Translation
An MCA stroke usually means blood flow is blocked in the area supplied by the middle cerebral artery, most often from a clot.
The MCA has several sections and branches, so symptoms depend on where the problem happens. A smaller blockage may cause mild weakness or sensory changes. A larger blockage can cause major deficits, like severe one-sided weakness, vision loss, neglect, or serious trouble speaking and understanding language.
Bleeding can also affect this same area, but that is treated differently than a typical clot-based MCA stroke.
Related FreshRN Article 👉 Middle Cerebral Artery Overview for Nurses and Students: Branches, Blood Supply, and Stroke Patterns
Common MCA Stroke Symptoms
MCA stroke symptoms depend on which side of the brain is affected, how large the stroke is, and whether the blockage involves a small branch or a larger part of the middle cerebral artery.
Because the MCA supplies areas involved in movement, sensation, vision, language, attention, and awareness, MCA strokes can cause a wide range of symptoms. Some patients have obvious weakness and speech changes. Others may seem confused, impulsive, inattentive, or unaware that anything is wrong.
Common MCA stroke symptoms include:
- Weakness on one side of the body, usually affecting the face and arm more than the leg
- Facial droop on one side
- Numbness or decreased sensation on one side of the body
- Slurred or unclear speech, also called dysarthria
- Difficulty speaking, understanding speech, reading, or writing, also called aphasia
- Vision loss on one side of the visual field, also called homonymous hemianopia
- Eyes looking toward one side, especially with larger MCA strokes
- Difficulty swallowing, which increases aspiration risk
- Confusion, decreased alertness, or altered level of consciousness
- Poor awareness of deficits, such as denying that the weak arm belongs to them or insisting they are fine when they are clearly impaired
- Neglect, where the patient does not notice or respond to one side of their body or environment
- Impulsivity, poor safety awareness, or unusual behavior
The side of the stroke matters.
A left MCA stroke usually affects the right side of the body. Because the left hemisphere is the dominant language hemisphere for most people, left MCA strokes commonly cause aphasia. Aphasia is a language problem, not just a speech problem. The patient may have trouble getting words out, understanding what others are saying, naming objects, reading, writing, or following commands.
A right MCA stroke usually affects the left side of the body. Right MCA strokes are more likely to cause neglect, poor spatial awareness, impulsivity, and poor insight into deficits. These patients may ignore the left side of their body, leave food untouched on the left side of the tray, run into objects on the left, or try to get up even though they are not safe to walk.
A helpful bedside distinction is this:
Dysarthria means the patient has trouble physically producing clear speech. Their words may sound slurred, weak, or garbled, but their language processing may still be intact.
Aphasia means the patient has trouble with language itself. They may not understand speech, may not be able to find the right words, or may produce speech that does not make sense.
For nurses, the key is to look beyond “Can they talk?” and assess the full pattern: face, arm, leg strength, sensation, vision, speech clarity, language comprehension, attention, swallowing safety, awareness of deficits, and changes from baseline.
Types of Strokes That Can Affect the MCA
Ischemic Stroke (most common by far)
An ischemic stroke occurs when a blood clot blocks blood flow through an artery supplying the brain. In the case of an MCA stroke, the blockage happens in one of the branches of the middle cerebral artery, cutting off oxygen to key brain regions.
Common causes include:
- Atherosclerosis (plaque buildup in the arteries)
- Cardioembolic events (clots traveling from the heart, often due to atrial fibrillation)
- Small vessel disease from hypertension or diabetes
If blood flow isn’t restored quickly, brain cells begin to die, causing motor, sensory, language, or cognitive impairments, depending on the MCA territory involved, requiring emergency treatment.
Emergency treatment may include IV thrombolytic therapy and/or mechanical thrombectomy when the patient meets eligibility criteria. Eligibility depends on last-known-well time, imaging findings, stroke severity, contraindications, and whether a large-vessel occlusion is present.
Hemorrhagic Stroke
A hemorrhagic stroke results from the rupture of a blood vessel, leading to bleeding into or around the brain.
Hemorrhage affecting the MCA territory may occur from intracerebral hemorrhage, hemorrhagic transformation of an ischemic infarct, or rupture of an MCA aneurysm or AVM. These are managed differently from ischemic MCA strokes, so nurses should avoid assuming every MCA-pattern deficit is treated with thrombolytics.
- The bleeding compresses adjacent brain tissue, which raises intracranial pressure and disrupts normal brain function.
- High-risk patients often have:
- Uncontrolled hypertension
- Known or undiagnosed aneurysms or AVMs
- History of head trauma
- Blood vessel wall fragility (e.g., from smoking or connective tissue disorders)
- Treatment may include blood pressure control, neurosurgical intervention, or neuro ICU-level monitoring to reduce secondary brain injury.
Transient Ischemic Attack (TIA)
A transient ischemic attack (TIA) is a transient episode of neurologic dysfunction caused by focal ischemia without evidence of acute infarction. Symptoms often resolve within minutes, but the resolution of symptoms does not automatically prove it was “only” a TIA. Patients still need urgent evaluation because early stroke risk is highest soon after a TIA. It’s a 🚩 major red flag 🚩 that a full stroke may occur soon.
A TIA in the MCA territory may cause brief symptoms like:
- Weakness or numbness on one side
- Difficulty speaking
- Temporary vision changes
Even though the effects go away, a TIA should always be evaluated and treated immediately to prevent a future stroke. Think of it as a loud warning bell 🛎️ (more on that later).
MCA Aneurysms
An MCA aneurysm is an abnormal bulge or ballooning in the wall of the middle cerebral artery. MCA aneurysms often develop near areas where the artery branches, especially around the MCA bifurcation.
Many MCA aneurysms are unruptured and may not cause symptoms. Some are found incidentally on imaging done for another reason. Others may cause symptoms if they press on nearby brain tissue or cranial nerves, though many remain silent until they rupture.
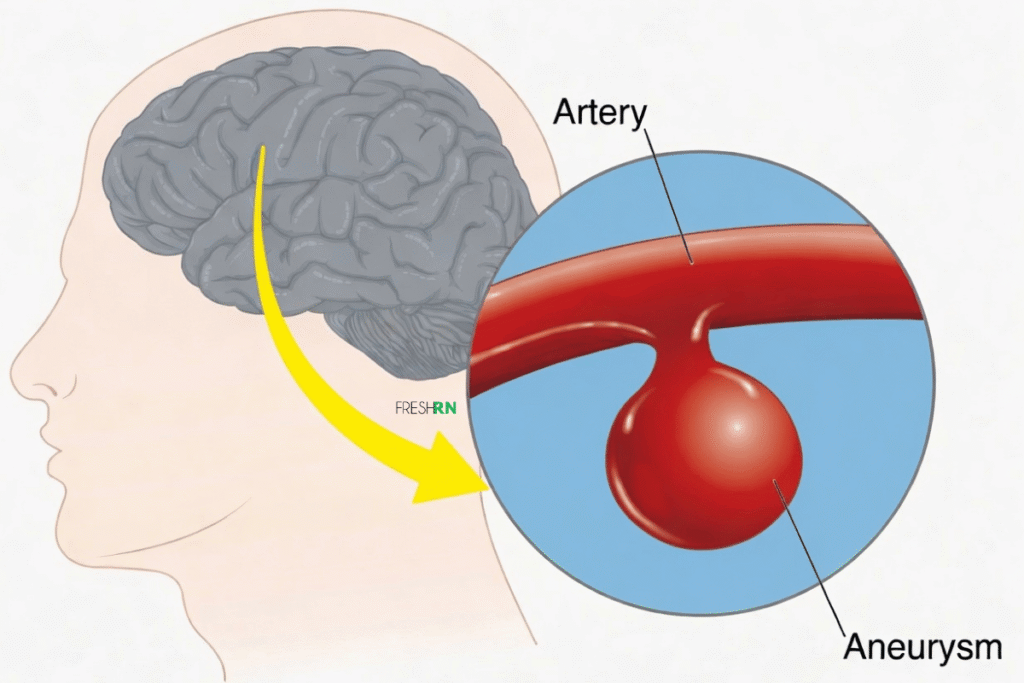
The major concern with any cerebral aneurysm is rupture. When an MCA aneurysm ruptures, it usually causes bleeding into the space around the brain, called a subarachnoid hemorrhage. This is a neurologic emergency.
Symptoms of a ruptured MCA aneurysm may include:
- Sudden, severe headache, often described as the worst headache of the patient’s life (or described as a “thunderclap.”)
- Nausea and vomiting
- Neck stiffness
- Sensitivity to light
- Altered level of consciousness
- Confusion or agitation
- Seizure
- New neurologic deficits, such as weakness, facial droop, speech changes, or vision changes
- Sudden collapse or loss of consciousness
A ruptured MCA aneurysm is different from a typical ischemic MCA stroke. In an ischemic stroke, blood flow is blocked. With a ruptured aneurysm, bleeding is the problem. These patients may still have MCA-pattern deficits, but the treatment priorities are different.
Treatment depends on whether the aneurysm is ruptured or unruptured, the size and shape of the aneurysm, the patient’s condition, and the anatomy of the blood vessels. Treatment may include close monitoring, blood pressure management, seizure management when indicated, reversal of anticoagulation when appropriate, and definitive aneurysm repair.
Definitive treatment for MCA aneurysms may involve surgical clipping or an endovascular procedure, such as coiling or stent-assisted treatment. MCA aneurysms are often considered for surgical clipping because of their branching anatomy, but the best approach depends on the individual aneurysm and the treating neurosurgical or neurointerventional team.
Nursing care after a ruptured MCA aneurysm focuses on close neurologic monitoring and preventing secondary brain injury. These patients may be monitored for complications such as:
- Rebleeding
- Vasospasm
- Delayed cerebral ischemia
- Hydrocephalus
- Increased intracranial pressure
- Seizures
- Electrolyte abnormalities, especially sodium changes
- Fever
- Aspiration
- Decreased level of consciousness
🔑 Key point for RNs: an MCA aneurysm can produce MCA-type neurologic symptoms, but it is not managed the same way as an ischemic MCA stroke. Sudden severe headache, collapse, seizure, or rapid decline should raise concern for hemorrhage and requires immediate escalation.
What Can Go Wrong After an MCA Stroke?
MCA strokes can change quickly, especially in the first few hours to days. Some patients look stable at first and then worsen as swelling increases, bleeding develops, or complications appear. This is why frequent neuro assessments matter.
Nurses are not just watching “stroke symptoms.” They are watching for secondary brain injury, airway problems, aspiration, immobility complications, and subtle signs that the patient is getting worse.
Common complications after an MCA stroke include:
Cerebral Edema and Increased ICP
A large MCA stroke can cause significant brain swelling. This swelling may increase intracranial pressure, shift brain tissue, and reduce blood flow to nearby areas.
Signs of worsening cerebral edema or increased ICP may include:
- Decreased level of consciousness
- New or worsening confusion
- Worsening weakness
- New pupillary changes
- Headache
- Vomiting
- New gaze deviation
- Cushing’s response: widening pulse pressure, bradycardia, and irregular respirations
- Seizure
- Posturing
- Sudden neurologic decline
This is one reason serial neuro assessments are so important. A small change may be the first sign that the brain is swelling.
Malignant MCA Syndrome
A severe MCA stroke can lead to malignant MCA syndrome, which is massive swelling after a large MCA infarct. This is a life-threatening complication.
As swelling increases, the brain can shift across the midline and compress important structures. These patients may deteriorate rapidly and may require aggressive management, including hyperosmolar therapy, ICU care, airway support, or decompressive hemicraniectomy. (Patients with this would require neuro ICU/ICU level of care.)
Nurses should be especially concerned when a patient with a large MCA stroke becomes increasingly drowsy, harder to arouse, more confused, or develops worsening neurologic deficits.
Hemorrhagic Transformation
An ischemic stroke can sometimes convert into an area of bleeding. This is called hemorrhagic transformation. It is more likely with larger infarcts and may also occur after reperfusion therapies, though many factors affect risk.
Possible signs include:
- Sudden neuro decline
- New or worsening headache
- Nausea or vomiting
- Acute blood pressure changes
- Worsening weakness, speech changes, or level of consciousness
- Seizure
Any sudden decline after an ischemic stroke should be escalated quickly.
Airway and Respiratory Compromise
MCA strokes do not usually damage the brainstem respiratory centers directly, but they can still threaten airway safety.
This can happen because of:
- Decreased level of consciousness
- Vomiting
- Poor secretion management
- Dysphagia
- Weak cough
- Aspiration
- Seizure
- Worsening cerebral edema
A patient who is becoming less alert is also becoming less able to protect their airway. Neuro decline and airway risk often go hand in hand.
Aspiration and Pneumonia
MCA strokes can impair swallowing, alertness, facial strength, tongue control, cough strength, and secretion management. This puts the patient at risk for aspiration.
Aspiration can happen with food, fluids, saliva, vomit, or oral secretions. It may be obvious, such as coughing or choking, but it can also be silent.
Nursing priorities include:
- Keep the patient NPO until an approved swallow screen is completed
- Follow speech therapy recommendations closely
- Watch for coughing, wet voice, drooling, pocketing food, or delayed swallowing
- Maintain good oral care
- Monitor for fever, increased oxygen needs, lung sound changes, or respiratory decline
Aspiration pneumonia can significantly worsen recovery and should be taken seriously.
Seizures
Cortical strokes, including many MCA strokes, can increase seizure risk. Seizures may occur early after the stroke or later in recovery.
Seizure activity may be obvious, but it can also be subtle. Watch for:
- Rhythmic jerking
- Eye deviation
- Sudden unresponsiveness
- Repetitive movements
- Sudden confusion or agitation
- Unexplained decline in mental status
- New incontinence
- Postictal drowsiness
Suspected seizure activity after a stroke requires prompt escalation.
Falls and Injury
MCA stroke patients can be at high risk for falls, especially when they have weakness, neglect, impulsivity, poor insight, visual field loss, or poor balance. Remember, strokes are sudden.
Right MCA strokes can be particularly tricky because patients may not recognize how impaired they are. A patient may insist they can walk even when they cannot safely sit, stand, or attend to one side of the room. Imagine being completely normal one moment, then the next, you’ve got profound weakness on your left side. It is reasonable that a patient will overestimate their capabilities when attempting to move or change positions independently.
Fall prevention is not just a checkbox. It is active stroke care.
DVT and Pulmonary Embolism
Weakness and decreased mobility increase the risk of venous thromboembolism. Stroke patients may not move the affected side well, may spend long periods in bed, and may not be able to communicate pain clearly.
Nursing priorities include:
- Apply ordered DVT prophylaxis
- Use SCDs correctly when ordered
- Encourage safe mobility as soon as appropriate
- Monitor for unilateral leg swelling, warmth, redness, pain, unexplained tachycardia, chest pain, or shortness of breath
A pulmonary embolism can be catastrophic in a patient already recovering from a major neurologic injury.
Shoulder Subluxation and Pain
Arm weakness after an MCA stroke can lead to shoulder subluxation, pain, and injury. The affected arm should not be pulled during repositioning, transfers, or boosting.
Nursing priorities include:
- Support the affected arm during positioning
- Avoid pulling on the weak arm
- Use safe transfer techniques
- Watch for shoulder pain, swelling, decreased range of motion, or guarding
- Involve PT and OT early
Protecting the affected shoulder matters because pain can limit participation in rehab.
Skin Breakdown
Weakness, immobility, decreased sensation, incontinence, poor nutrition, and altered mental status all increase skin breakdown risk.
Patients may not feel pressure normally or may not be able to reposition themselves. Neglect can make this worse because the patient may not recognize one side of the body as needing attention.
Nursing priorities include frequent repositioning, skin checks, moisture management, nutrition support, pressure injury prevention, and careful attention to the affected side.
Depression, Emotional Lability, and Cognitive Changes
Stroke recovery is not only physical. Patients may experience depression, anxiety, emotional lability, personality changes, frustration, fatigue, poor attention, memory problems, and impaired judgment. While depression and anxiety can take time to develop, we may observe more sudden changes at the bedside shortly after the event occurs. This can be shocking to family members (for example, the mild-mannered pastor of 40 years is cursing up a storm), or you may encounter behavior that is difficult to manage at the bedside (such as impulsivity).
After any neurological event, it’s critical for the nurse to observe these changes and communicate with the family. Often, I tactfully asked whether what we’re seeing at the moment is consistent with behavior at home to ensure an accurate assessment. Some patients are impulsive at home, while others are not. You may observe patients who are often very tearful and outwardly emotional with loved ones, but the patient is very stoic, and they’ve never seen them cry before.
These changes can affect participation in therapy, safety awareness, family dynamics, and long-term recovery.
It’s critical for the RN to notice these changes early because they spend the most time watching how the patient behaves across the shift, rather than a shorter, isolated visit by a neurologist.
Why This Matters for Nurses
After an MCA stroke, the nurse’s job is not only to document deficits. The nurse is watching for patterns and changes.
A patient who is more drowsy than before, coughing after sips of water, ignoring one side of the body, newly vomiting, suddenly more confused, or weaker than the last assessment is telling you something.
The safest mindset is 👉 This patient has a vulnerable brain. My job is to catch deterioration early, protect airway and swallowing safety, prevent complications, and escalate changes fast.
If you’re a new neuro nurse and giving report on stroke patients still feels overwhelming, you’re not alone. Grab my free 3-lesson email mini-course 👇 that walks you through exactly how to do it clearly and confidently.
MCA Stroke Nursing Diagnosis & Care
Nursing care provided after an MCA stroke focuses on stabilization, prevention of complications, and maximizing recovery. Let’s go through possible nursing diagnoses and a layman’s translation.
- Impaired physical mobility – can’t move as well as before, likely needs assistance
- Impaired verbal communication – can’t speak as well as before
- Sensory perception deficits – decreased or altered ability to feel, interpret, or respond to sensory input, such as light touch, pain, temperature, pressure, or body position.
- Risk for aspiration (especially with impaired swallowing) – they are at risk for choking on food and/or fluids; instead of it going down their food pipe (esophagus), it goes down their windpipe (trachea)
- Risk for injury (due to hemiparesis or altered LOC) – much more likely to hurt themselves doing normal things, like getting up to go to the bathroom or using utensils to eat, because they cannot control their body well, and/or it’s much more difficult to remain alert while engaging in regular activities (Example: Falling asleep in the chair and falling out of it).
- Deficient knowledge (related to new deficits or treatment plan) – a lot of complex medical terminology and situations are unfolding rapidly and it’s very difficult for them to really understand what’s going on
- Inability to care for self – due to all of these new difficulties and needs, the patient can no longer function independently (this is a really big one!)
A nursing care plan should prioritize:
- Maintaining the airway and oxygenation – MCA strokes do not usually damage the brainstem respiratory centers directly, but they can still threaten airway safety through decreased level of consciousness, impaired protective reflexes (like coughing/airway clearance), dysphagia, poor secretion management, vomiting, or aspiration.
- Monitoring neuro status closely – neuro changes are often subtle and can indicate decline
- Fall prevention strategies – these patients often have impaired balance, sensory perception, and can also be impulsive due to the changes in their brain; they’re major fall risks!
- Skin integrity, nutrition, and hydration – because of airway and swallowing changes, patients often need modified diets to eat safely, and they also typically have trouble moving themselves in bed to prevent skin breakdown
- Early involvement of speech, OT, and PT – the parts of their brain that dictate things like speech, movement, and balance are often impacted. Early PT, OT, and speech therapy help assess deficits, prevent complications, start safe mobility and swallowing plans, and support neuroplasticity and functional recovery.
- Emotional support for the patient and family – strokes are sudden and scary; the patient may have been functioning normally one minute, and the next cannot speak or move one side of their body, and are staring down the barrel of a very long recovery process with a life that looks totally different. It’s traumatic for the patient and family to endure; therefore, your emotional support as their primary caregiver is critical.
Neuro Assessments: The Gold Standard 🏆
The most important foundational aspect of effective nursing care for any stroke patient is patient assessments. In nursing, we often have a working assumption that if things are changing clinically with the patient, it will be evident in things like vital signs or patient report. However, neuro changes are subtle and often occur without the patient being actively aware of it. (Not to mention, some are unconscious!) Therefore, the way to assess for complications in your MCA stroke patients (and all stroke patients!) in patients is with repeated neuro checks.
(If you’re a nurse and want to get better at neuro checks, here’s a free resource to walk you through the process! 👇)
What Causes MCA Stroke?
MCA ischemic strokes are commonly embolic, often from the heart or large arteries such as the carotids, but they can also result from intracranial atherosclerosis, local thrombosis, small-vessel disease affecting deep perforators, dissection, hypercoagulability, or less common vasculopathies.
The vast majority of strokes are associated with identifiable risk factors. According to the INTERSTROKE study, ten modifiable risk factors account for approximately 90% of the population-attributable risk of stroke worldwide [SOURCE]. Let’s go through some risk factors and why it puts a patient at a higher risk.
MCA Stroke Risk Factors
Carotid artery disease ➡️ The large blood vessels to your brain are getting clogged, making it easier for a blockage to cut off blood flow and cause a stroke.
Atrial fibrillation ➡️ When your heart beats irregularly, it can’t fully contract and empty all the blood from its chambers. Blood pools inside the heart and forms clots. These clots can break off, travel to the brain, and cause a stroke. This is why anticoagulants (blood thinners) are a standard treatment for AFib.
Hyperlipidemia (high cholesterol) ➡️ Too much cholesterol in your blood builds up as plaque on the walls of your arteries. This narrows the vessels and makes clots more likely, blocking blood flow to the brain and causing a stroke.
Smoking ➡️ Smoking damages blood vessels and makes blood thicker and stickier, which raises the chance of clots forming and causing a stroke.
Hypertension ➡️ Long-term high blood pressure damages and weakens your blood vessel walls over time. This greatly increases your risk of stroke, most often by causing blockages or clots. In rare cases, it can cause a brain vessel to rupture.
Diabetes ➡️ Consistently high blood sugar damages the blood vessels themselves. It also makes the blood thicker (higher viscosity), so it clots more easily and quickly, greatly raising your risk of stroke.
Just having one or two of these can significantly increase the risk of having more, let alone having more than that. Stroke prevention is an important thing to educate patients and families about.
The Strongest Predictor of a Stroke
A prior stroke or TIA is one of the strongest predictors of future stroke. For modifiable risk, hypertension remains the biggest target. Some studies indicate that up to 1 in 4 stroke survivors will have another stroke within 5 years. The point of contact while a patient is in the hospital recovering from a stroke is key to educating them to prevent another stroke.
Final Thoughts: MCA Stroke Takeaways
MCA strokes are common, serious, and can lead to wide-ranging deficits depending on the affected brain region. Nurses play a crucial role in supporting patients through acute care, rehabilitation, and long-term recovery. Early recognition, fast treatment, and coordinated care can significantly improve outcomes.
More Resources on Strokes
- Why is My Stroke Patient NPO? What To Do & Why
- Nursing Priorities for Ischemic Stroke Patients – From a Neuro Nurse
- S2E21: Code STEMI, Code Stroke, and Code Sepsis
- Middle Cerebral Artery Overview for Nurses and Students: Branches, Blood Supply, and Stroke Patterns
- Left MCA Strokes: What Happens With Strokes Involving the Left Middle Cerebral Artery
- Want more general tips for starting out in neuro? Check out my popular video: Tips for New Neuro Nurses (58K+ views)
Wish you had a guide for your first neuro nursing job? Here it is!

Neuro is a specialty that can feel intimidating at first. There’s a ton of new terminology, patient conditions can change fast, and neuro assessments are way more nuanced than they seem. It’s a lot to take in—but you don’t have to figure it out alone. Neuro Wise is the course we wish we had as new neuro nurses. It breaks down complex neuro concepts into easy-to-understand lessons, so you can confidently assess your patients, give a solid neuro report, and actually understand what’s going on—not just go through the motions. We cover everything you need to know—so you can step onto the unit feeling prepared, not panicked.
Click for Instant Access



0 Comments